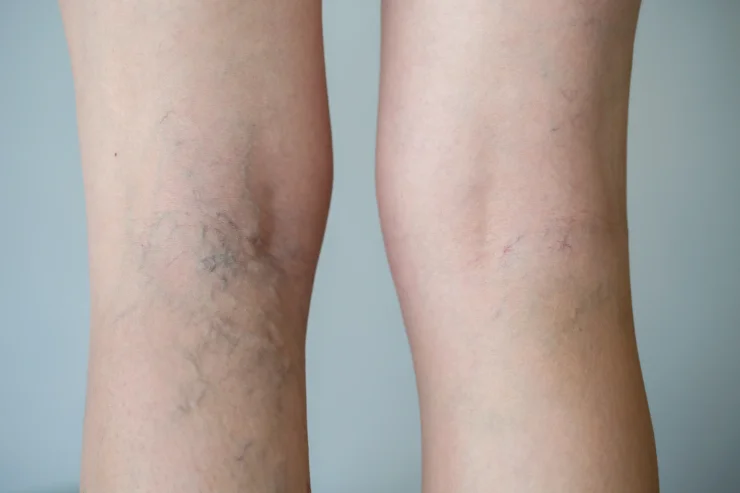
There are two sets of risk factors for varicose veins: Those you can control and those that you can’t.
Unfortunately, some of the major risk factors include your sex, family history, and age. People over age 50 are at a higher risk for developing spider veins, and menopause also increases your risk factor (6).
The good news, though, is that there are certain lifestyle factors that ramp up your risk—and those are things we can change!
1. Sedentary Lifestyle
The more you sit for prolonged periods of time, the higher your risk factor for varicose veins. When you sit for too long, it can cause blood to pool in the veins in your legs—the very thing we want to avoid. Break up long periods of sitting still with daily walks, leg day at the gym, or even stretches from the couch (7)!
2. Standing for Too Long
On the other side of the coin, standing for too long can also pose a risk. This is especially an issue for people whose jobs require them to stand in a mostly stationary spot for several hours each shift (8). The blood in your legs simply doesn’t flow as well when you’re still, whether you’re standing or sitting.
To help mitigate this, take short walk breaks every 45 minutes. If you can’t take breaks while standing, try doing squats in place, leg lifts, or simple stretches—anything to get that blood flowing.
3. Obesity
If you’re carrying extra weight, there may be extra pressure on your veins that can increase your risk factor (9). Since switching up your diet and moving more are solutions to many other spider vein risk factors, you may find yourself losing weight from habit change alone without even realizing it.