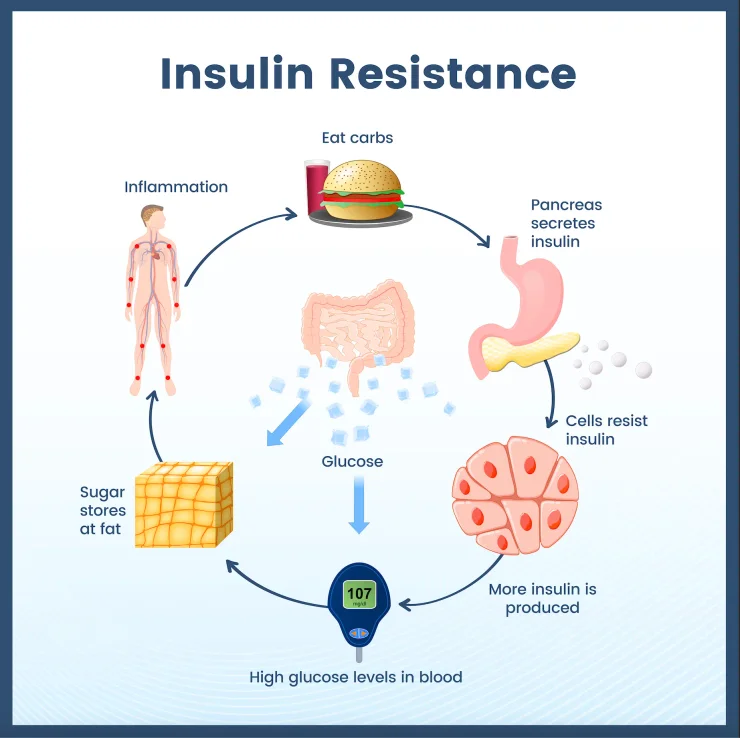
Insulin resistance can often be reversed through a series of lifestyle
changes. One of the most common solutions is a low-carb diet (29, 30).
Since your body gets blood sugar from carbs, reducing the number of carbs
you eat reduces the amount of blood sugar you’re taking in. In fact, if
you’re really into this idea, you can take your low-carb diet to
the next level and try the keto diet.
On the keto diet, you reduce your carb intake to the extent that your body
must switch over from using blood sugar as energy to using fat as energy (31). When this happens, it means your body is in ketosis. Studies have found
that ketosis can fully reverse insulin resistance (32, 33, 34). It can also help you lose weight and feel more full (35)!
Other ways to reduce or reverse insulin resistance include getting regular
exercise, reducing how much sugar you eat, quitting smoking, eating whole foods, taking omega-3s, getting better sleep, and managing your stress (36, 37, 38, 39, 40). Along with reducing insulin resistance, habits like these can lead to an
overall happier, healthier, and calmer lifestyle.